CMO,
Healthcare Finance Group
The Delivery System Reform Incentive Payment (DSRIP) program is an outgrowth of the Accountable Care Act, which directed the Department of Health and Human Services to issue regulations increasing the transparency of the Medicaid Section 1115 waiver approval and renewal process. Proposed regulations were released in September 2010, and since then seven states have begun implementing the Medicaid focused program.
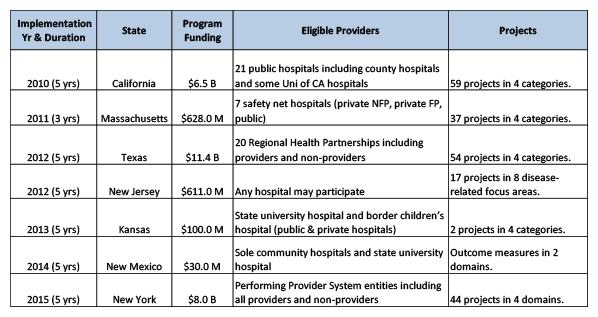
The three largest programs, each with more than $5 billion in funding, are in California, Texas and New York. Interestingly, the California program was focused on public hospitals, while the Texas program included several provider types and some non-providers. The New York program, effective in April 2015, will be open to all healthcare providers and non-providers. The evolution to include more provider types and non-providers, in conjunction with extremely broad-based New York program initiatives, may lead other states to expand programs, turning the DSRIP program into a catalyst for healthcare delivery system change — which may directly or indirectly affect ABLs lending into the industry.
Federal Goals
DSRIP is an optional federal Medicaid waiver program implemented at the state level for states with high Medicaid expenses, created to redirect Medicaid and supplemental dollars currently only available to hospitals as a reward to healthcare providers for improving quality and containing costs. Upon obtaining a Medicaid Section 1115 waiver,1 states can reward providers for implementing successful delivery systems and payment reform projects. The projects must align with the Centers for Medicare & Medicaid Services’ (CMS) general goals of integrating healthcare systems within different regions, moving from “fee for service” to “fee for quality,” and creating care coordination across a population. By not defining successful implementation and specific project details, CMS forces states to make those decisions. CMS believes that each state is better placed than the federal government to design the individual programs.
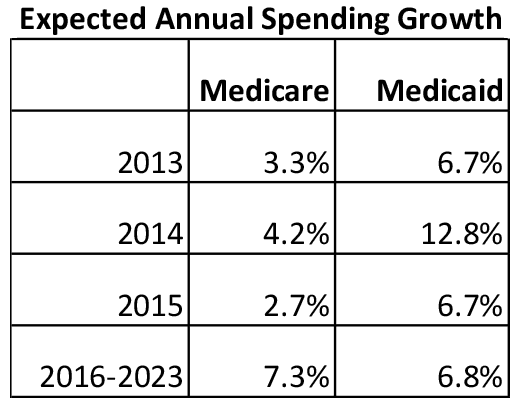
CMS established the DSRIP program to address the overall level of healthcare spending in the country and the costs associated with the so-called “Medicaid Super-Utilizers.” DSRIP’s goal is to reduce the expected increases in overall healthcare spending and, in particular, reduce the federal healthcare expenditures. Exhibit 12 summarizes the expected annual rates of growth in Medicare and Medicaid spending which CMS is endeavoring to reduce.
DSRIP’s second goal is to reduce costs associated with the Medicaid Super-Utilizers. These beneficiaries have “complex, unaddressed health issues and a history of frequent encounters with health care providers…patients who accumulate large numbers of emergency department visits and hospital admissions which might have been prevented by early interventions and primary care.”3 CMS’ presumption is integrating healthcare delivery will reduce costs and improve care quality for this population. While data from studies of Accountable Care Organizations (ACO) do not clearly support this claim, there is a generally accepted view that earlier intervention and more consistent follow-up care should reduce hospital admissions, which should reduce costs and improve quality.
Lender Implications
Though well-intended, one side effect of the DSRIP program may be the possible acceleration of the healthcare industry’s trend toward consolidation and affiliation, which has implications for lenders. Lenders supporting smaller independent healthcare providers ultimately could find fewer — and weaker — borrowers than newly formed, larger entities, creating a need for more innovative loan parameters. Lenders may also need unique structures to meet demand for loans supporting information technology projects, new and loosely formed joint ventures, and other non-traditional legal entities.
Generally, DSRIP programs are implemented over a five-year period, so the potential benefits to providers only become evident over time. During implementation, lenders may be challenged to find tangible proof of the program’s benefits, as the provider must front associated costs. The ABL could find itself over-advancing based on A/R-based revolving credit lines, only to discover that demand for these loans declines as newly formed, larger entities have access to less expensive financing, while smaller, independent entities are less able to support new loans. Other asset-based and cash-flow loans may also become more difficult to execute due to the complexity of the newly created organizations, requiring looser credit structures. That being said, significant hurdles exist to executing a DSRIP program, which is intended to only jumpstart a change in the healthcare landscape. So lenders will have time to adjust to the new landscape and determine how to best take advantage of the upcoming changes.
Participating States
The seven states in Exhibit 2 that have instituted a DSRIP program at the time of this writing, in order of implementation, are: California, Massachusetts, Texas, New Jersey, Kansas, New Mexico and New York. Each state’s Department of Health (DOH) agreed to be responsible for holding provider groups accountable for meeting program objectives; if objectives are not met, waiver payments are withheld. Under the oversight of each state’s DOH, several providers joined together to form a “DSRIP Entity.” The DOH determines if the entity is eligible to participate in the program, and approves projects and dollar goals.
Each of the seven participating states has interpreted this broad outline differently, making it hard to draw conclusions about the program’s effectiveness. And many hurdles remain to the program’s successful implementation. It is instructive to closely examine NY State — the most recent and comprehensive program to date.
NY State as a Roadmap
NY State established a Medicaid Redesign Team in 2011 to reform its healthcare system and reduce $50 billion in Medicaid spending. Its goal is to save $17.1 billion of Medicaid federal money over five years, using the DSRIP waiver program as a significant driver of savings. Specifically, the state established an $8 billion DSRIP program, with a potential total savings of $9.2 billion over the next 5 years. Money is allocated as follows:
| Pre-DSRIP for safety net providers4 | $500 Million |
| DSRIP Implementation, beginning April 1, 2015 | $6,420 Million |
| Medicaid Redesign for home health and long-term care | $1,080 Million |
| Potential Capital Restructuring Grants | up to $1,200 Million |
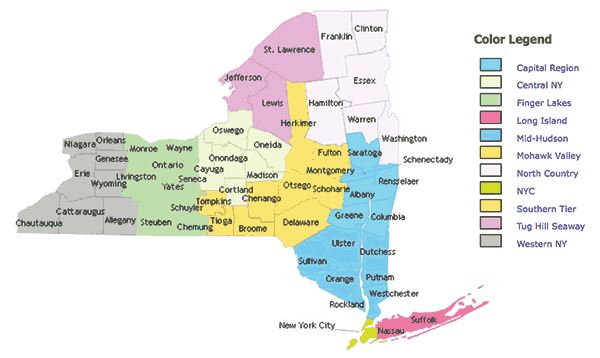
To qualify for participation in DSRIP, a provider or non-provider must join entities that together are defined as a Performing Provider System (PPS). Further, to be eligible to receive DSRIP money, the PPS must include several providers and provider types. The PPS must show evidence of being a Clinically Integrated Entity, which is reasonably expected to meet a region’s needs through the integration of care. The regions in Exhibit 3 were identified through NY State’s Community Needs Assessment, which analyzed population demographics. The 11 regions are significantly different in terms of population density, percentage of Medicaid beneficiaries and geography. The largest region is the sparsely
populated North Country, and the smallest, most densely populated is New York City. Not surprisingly, the number of so-called “Emerging PPS” entities eligible to participate in the state’s program varies widely. There is only one Emerging PPS in the North Country, and 14 in NYC. How the 14 Emerging PPS entities in NYC will work together to integrate healthcare services across the region will be highly instructive and indicative of the success of the program in other states.
NY State’s intention is to allocate funds based on three factors: the quality of the nearly 350- page application due December 22, 2014, the index score of the PPS’s projects and the number of allocated Medicaid beneficiaries. The index score is set by the DOH and based on the projected level of system transformation. Each PPS must collaborate on a minimum of five and a maximum of 11 projects in four different domains, or areas. The first domain relates to reporting on projects’ progress and is required by CMS. The other three domains relate to: (1) system transformation, such as home health at-risk intervention programs or expanding the use of telemedicine; (2) clinical improvement, such as the integration of primary care and behavioral health services; and (3) population-wide impact, such as programs to promote tobacco use cessation.
Scoring a PPS on its number of allocated Medicaid beneficiaries points to a potential challenge in forming a PPS. Because every beneficiary can only be attributed to one PPS, competition may exist between providers to “own” that beneficiary. While the program’s goal of rewarding collaboration is an effective mechanism to support sharing information and aligning goals, any competition for beneficiaries somewhat undermines the program’s intentions.
Implementation Hurdles
Other hurdles exist to establishing a program. The first relates to existing healthcare regulations, and the second pertains to governance of a DSRIP entity. NY State announced it will waive and modify regulations to achieve DSRIP’s goals, and reduce obstacles for providers seeking to join a PPS. Anti-trust regulations will be waived by issuing Accountable Care Organization Certificates and Certificate of Need requirements, and integration of services and space regulations will also be foregone. Other regulations to be modified include governance over patient transfers, the definition of long-term care patients and limitations on the number of observation beds. However, federal regulations remain in place, which may lead to conflicts between state and federal law.
Establishing an effective governing system is the second major hurdle to implementing a DSRIP program, and one that NY State’s PPS entities now face. For guidance, several NY State PPS entities are reviewing programs in California and Texas. California’s initiative started in 2010 and ends in 2015, and the University of California published a mid-point report in July 2014 on findings. A major conclusion is that the PPS entities need to establish better governance, and the state needs to create stronger channels of communication among participating health systems, as well as between health systems and state and federal partners. Texas started its $11.4 billion program in 2012 and established 20 regions. Perhaps, in part due to the experience of California, Texas assigned an anchor partner to each PPS to provide leadership and be the focal point for all communication between the PPS and the state. The report from Texas’ Region 10 Health Partnership Statewide Learning Collaborative found it should have spent more time studying how to promote collaboration and information-sharing among market competitors before implementing projects. These findings justify NY State’s concerns over how to effectively manage and govern a PPS.
Establishing, merging or aligning governing bodies is always challenging; when the players include previous competitors with entrenched leadership, it can be almost impossible. For this reason, PPS entities that have a highly centralized decision-making process and strong lead provider are most effective. Even with a strong lead, contentious issues and questions persist. For example: Should member roles and power be defined by their respective capital contribution, each member’s number of allocated beneficiaries, geographic coverage, provider type, or the number of projects a member agrees to undertake? How much data transparency is required? What are the rights of a participant if an entity is sanctioned as a poor performer? These issues can divert attention away from the overall effort, and may jeopardize implementation.
A New Vision
Despite the fact that the DSRIP waiver program is a major federal initiative to reduce Medicaid healthcare spending and move providers toward improving healthcare quality, few states have participated. However, the program is evolving, and Alabama, New Hampshire and Illinois are in various stages of developing DSRIP initiatives. If, over time, NY State’s PPS entities can overcome the challenges of governance and regulation, and are judged to be successful in reducing costs and improving the quality of care, the state’s program will provide important lessons for other states. In particular, the NY version of DSRIP opens the door to privately owned entities, which were previously blocked in the state. The resulting public-private partnerships and joint ventures might require lenders to adjust their approaches to lending into the sector.
To the extent the DSRIP program takes hold in multiple states, lenders will need to understand the different programs and know which providers are acting as DSRIP Entity leaders. They will also want to position themselves to take advantage of the newly forming groups, and stay abreast of legal changes. The dislocation of provider systems due to DSRIP programs is an opportunity and challenge for lenders that need to be nimble in the healthcare marketplace.
Claudia Gourdon is chief marketing officer at Healthcare Finance Group, LLC.
Footnotes:
1. Medicaid Section 1115 waivers are Research & Demonstration Project waivers. States apply for program flexibility to test new or existing approaches to financing and delivering Medicaid.↩
2. Data from CMS Office of the Actuary; Sept. 16, 2014. The 12.8% growth in 2014 reflects the ACA’s impact on enrolling the previously uninsured into the Medicaid programs.↩
3. CMS Information Bulletin: Targeting Medicaid Super-Utilizers to Decrease Costs and Improve Quality. July 24, 2013.↩
4.Funded through NY State’s Interim Access Accessibility Fund.↩